What Telemedicine, Telehealth Resource Centers Offer to Providers
The National Consortium of Telehealth Resource Centers, consisting of 2 national and 12 regional centers, offers a ready-made resource for telemedicine guidance.
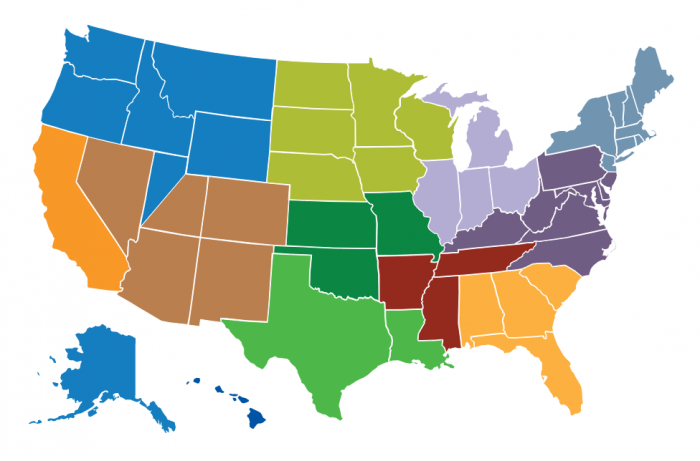
Source: Photo courtesy NCTRC
Healthcare providers, organizations and vendors interested in knowing more about telemedicine and telehealth have a ready resource at their fingertips: a network of telehealth resource centers covering every region of the country.
Established in 2006, the Regional Telehealth Resource Center (RTRC) Program consists of 12 regional and two national telehealth resource centers. The centers are funded by three-year renewable grants from the U.S. Department of Health and Human Services’ Health Resources and Services Administration (HRSA) Office for the Advancement of Telehealth (OAT), which is part of the Office of Rural Health Policy.
Together, they form what’s called the National Consortium of Telehealth Resource Centers (NCTRC).
The mission statements for the TRCs consist of:
- Providing technical assistance, training (including travel expenses) and support for healthcare providers and entities planning or providing telehealth services
- Disseminating information or research findings related to telehealth services
- Supporting effective collaboration among telehealth resource centers
- Conducting evaluations to determine the best utilization of telehealth technologies to meet healthcare needs
- Supporting the integration of technologies used in clinical information systems with other telehealth technologies
- Fostering the use of telehealth technologies to provide healthcare information and education for health care providers and consumers in a more effective manner
- Implementing special projects or studies
Dig Deeper:
In the Northeast, Telehealth Gets Creative - With Good Results
Telehealth Partnerships Focus on Innovative ROI in Upstate NY

Source: ThinkStock
NATIONAL RESOURCE CENTERS FOR TELEMEDICINE AND TELEHEALTH
The NCTRC includes two national centers.
The Center for Connected Health Policy, created and funded by the California Health Care Foundation, is based in Sacramento.
Launched in 2008 as a project of the Public Health Institute, the CCHP originally focused on California telehealth policy, and was credited with drafting the Telehealth Model Statute Report, which became the basis for the California Telehealth Advancement Act of 2011 (AB 415). In 2012, the CCHP formally became the federally designated National Telehealth Policy Resource Center (NTRC-P).
The CCHP is described as “an independent center of excellence in telehealth policy providing technical assistance to twelve federally funded telehealth regional resource centers.”
Its goal is to “encourage collaboration among policy makers, researchers, industry leaders, health advocacy organizations and other influential groups to advance telehealth policy solutions at the state and federal levels.”
The CCHP “assists RTRCs in responding to regional policy challenges by providing relevant policy information, resources, training and technical assistance and keeps the public abreast of emerging policy issues,” its website states.
One of CCHP’s most popular resources is the State Telemedicine Laws and Reimbursement Policies, an annual report on state legislation relating to telemedicine and telehealth and Medicaid reimbursement policies.
Among the CCHP’s current projects are an analysis and impact study on telehealth private payer laws and a roadmap for eConsult sustainability.
The National Telehealth Technology Assessment Resource Center (TTAC), based out of the Alaska Native Tribal Health Consortium (ANTHC), is located in Anchorage, Alaska. It serves as a tech resource for healthcare providers.
The TTAC’s key objectives are:
- Raising awareness of national standards surrounding telehealth and telemedicine technologies;
- Facilitating the development of a national policy and guidance for the regional TRCs;
- Working with national organizations on the development of industry-wide technology standards; and
- Collaborating with the regional TRCs and national experts on policy.
The TTAC, which is funded by the ANTHC and HRSA grants, “aims to create better-informed consumers of telehealth technology,” its website states. The center offers a number of resources, including toolkits, videos, webinars and guidance documents focusing on the technology behind telehealth and telemedicine programs and implementations.
Garret Spargo, the TTAC’s principal investigator and a 12-year veteran in the telemedicine and telehealth industry, says the center’s goal is to help healthcare providers become comfortable with the technology they need and use.
Oftentimes a health system might take on too much new technology, or administrators may feel they need all the latest bells and whistles to create an effective program, when in fact the simplest platforms are the ones that work best.
Speaking at a regional conference hosted by the NorthEast Telehealth Resource Center in Amherst, Mass., Spargo said telemedicine technology is constantly evolving, and that providers should look to co-opt and customize what’s available to them.
“Make it your own,” he said. “Make it work for you.”
That’s where the toolkits come into play. Described as “interactive elements [that] allow users to learn the fundamentals of how various technologies work, as well as how to assess them for use in telehealth programs,” the TTAC has unveiled more than 25 toolkits, on everything from video conferencing platform to Google Glass.
- Another resource often mentioned in the same breath as the TRC network is the Center for Telehealth & eHealth Law (CTeL). Launched in 1995 by a consortium including the Mayo Foundation, Cleveland Clinic Foundation, Texas Children's Hospital and the Mid-West Rural Telemedicine Consortium, CTeL is a Washington D.C.-based non-profit organization that focuses on compiling, analyzing and disseminating information on legal and regulatory issues associated with telemedicine, including licensure and reimbursement.
Dig Deeper:
Examining the State of Medicaid Telehealth Reimbursement
Is There a Difference between Telemedicine and Telehealth?

Source: ThinkStock
REGIONAL TELEHEALTH RESOURCE CENTERS
There are currently 12 resource centers scattered across the country, covering every state and affiliated Pacific islands. They are:
- The TexLa Telehealth Resource Center, based in Lubbock, Texas and covering all of Texas and Louisiana
- The Mid-Atlantic Telehealth Resource Center (MATRC), based at the University of Virginia Center for Telehealth in Charlottesville and covering Pennsylvania, New Jersey, Delaware, Maryland, Virginia, West Virginia, Kentucky, North Carolina and Washington D.C.
- The Upper Midwest Telehealth Resource Center (UMTRC), a consortium of active telehealth organizations based with the Indiana Rural Health Association in Terre Haute and covering Indiana, Illinois, Michigan and Ohio
- The Southeastern Telehealth Resource Center (SETRC), based in Blackshear, Ga., consisting of the Alabama Partnership for Telehealth, Florida Partnership for Telehealth, Georgia Partnership for Telehealth and the worldwide non-profit Global Partnership for Telehealth and covering Alabama, Florida, Georgia and South Carolina
- The Pacific Basin Telehealth Resource Center (PBTRC), based at the University of Hawaii in Manoa and covering Hawaii and the Pacific Basin
- The Heartland Telehealth Resource Center (HTRC), based at the University of Kansas in Lawrence, consisting of the University of Kansas Center for Telemedicine and Telehealth, the Missouri Telehealth Network, the Telehealth Alliance of Oklahoma and the University of Oklahoma Health Sciences Center and covering the states of Kansas, Missouri and Oklahoma
- The South Central Telehealth Resource Center (learntelehealth.org), based at the University of Arkansas for Medical Sciences Center for Distance Health in Little Rock and covering Arkansas, Mississippi and Tennessee
- The Southwest Telehealth Resource Center (SWTRC), based with the Arizona Telemedicine Program at the University of Arizona Health Sciences Center in Tucson and covering Nevada, part of Utah, Colorado, Arizona and New Mexico
- The Northwest Regional Telehealth Resource Center (NRTRC), based at the Utah Telehealth Network at the University of Utah in Salt Lake City and covering 41 telehealth networks throughout Alaska, Washington, Oregon, Idaho, Montana, part of Utah and Wyoming
- The Great Plains Telehealth Resource and Assistance Center (gpTRAC), based at the University of Minnesota Institute for Health Informatics in Minneapolis and covering Minnesota, North and South Dakota, Iowa, Wisconsin and Nebraska
- The California Telehealth Resource Center (CTRC), based with the California Telehealth Network in Sacramento and covering 10 telemedicine networks and two learning centers (at the University of California campuses in Davis and San Diego) throughout California
- The NorthEast Telehealth Resource Center (NETRC), based with Medical Care Development’s Public Health Division in Augusta, Me., partnering with the University of Vermont Medical Center and covering Maine, Vermont, New Hampshire, Massachusetts, Connecticut, Rhode Island, New York and New Jersey
Most, if not all, telehealth resource centers offer a three-tiered approach to assisting healthcare providers.
TRC officials are available to answer, by phone or e-mail, basic questions about telehealth and telemedicine. At the next level, a TRC can offer up to 10 hours of free technical assistance per client per year (the client must complete a registration form). If that’s not enough, the health system can arrange a partnership with the TRC “for consultative services for additional, in-depth assistance requiring more than 10 hours.”
Telehealth resource centers “are basically there to help guide [healthcare providers] along,” says Andrew Solomon, project manager for the NETRC. “We’re there to answer any questions they have, and to point them in the right direction.”
Many TRCs also hold annual regional summits, or partner with other TRCs or organizations like regional Rural Health Associations to host a telehealth- or telemedicine-based conference. They’re also present in the Exhibit Hall at the American Telemedicine Association’s annual conference, and at events like the annual conference of the American Academy of Family Physicians.
A new organization created by the TRC network is the Society for Education and the Advancement of Research in Connected Health (SEARCH), a telehealth research collective launched out of the South Central and Mid Atlantic TRCs in 2016. SEARCH held its first telehealth symposium this past April in Virginia and has a fall meeting planned for Oct. 5-6 in Philadelphia.
The reasoning behind SEARCH, says one of its organizers, is to create a national conversation on telehealth and telemedicine issues affecting the nation’s healthcare system as a whole.
“We’re looking for [health systems] to tells us what are the big-ticket telehealth items that you need to get answers to,” says Dr. Judd Hollander, Associate Dean for Strategic Health Initiatives at Sidney Kimmel Medical College and Vice Chair for Finance and Healthcare Enterprises in the Department of Emergency Medicine at Philadelphia’s Thomas Jefferson University. “A lot of them have questions … that aren’t being answered.”
Dig Deeper:
NETRC Conference: Telehealth on the Path to Mainstream Adoption
Making the Most Out of Telehealth

Source: ThinkStock
LOOKING TO THE FUTURE
Among the projects on the horizon are a national database of telehealth and telemedicine programs (tentatively called Telehealth Connect), telehealth leadership forums (NETRC recently launched one) and resources devoted to what officials say are up-and-coming concepts.
“Over the next three to five years, technologies for mHealth, population-based health and remote patient monitoring will dominate the telehealth and healthcare industry,” NCTRC officials said in a recent report commemorating the 10th anniversary of the founding of the TRC network.
“As these technologies gain more visibility and popularity, the TRCs will be able to provide an experienced, agnostic voice to help all participants in the health system make informed decisions. The uniqueness of the TRCs, regionalized specialization but working collaboratively together to provide a consistent, cohesive voice, positions them perfectly to deliver accurate, comprehensive information to the wide range of parties interested in telehealth.”
While the telehealth resource centers map out their futures based on the three-year HHS grant cycle, advocates hope they’ll be valuable enough to someday become permanent fixtures in the healthcare landscape. For now, they’re busy enough finding answers to those daunting telehealth and telemedicine questions that everybody seems to have.
Dig Deeper:
Direct-to-Consumer Telehealth: One Hospital’s Virtual Care Plan
In Value-Based Care, Telehealth’s Aim is Money Saved, Not Earned
