Telemedicine Robots: Out of Science Fiction and Into the Mainstream
Robots and robotics have been a fixture in healthcare for decades. New telehealth and mHealth tools are giving them a chance to shine.

Source: Thinkstock
- Long a staple of science fiction, robots are now proving their value as a telemedicine resource.
Originally designed to ferry supplies around the hospital or give surgeons a steadier hand for delicate medical procedures, robots are now finding their way into the care continuum, thanks to a variety of designs that can turn them into walking, talking healthcare kiosks. Healthcare robots can take orders from and deliver items to a patient, act as an around-the-clock sitter, assist frail and elderly patients out of a bed or chair, or provide a video connection to a distant doctor.
“There’s a lot of opportunity for this technology in healthcare,” says Daniel Theobald, Vecna’s Co-Founder and Chief Innovation Officer and a leading expert on robotics in healthcare. “If you look around now you’ll see them.”
Robots have proven especially helpful in telemedicine. Companies like VGo and InTouch have developed robots that serve as the doctor’s stand-in in remote clinics, community health centers, schools, cruise ships, sporting events, even smaller hospitals. They’ve even been used to provide home-bound or quarantined children with an avatar of sorts, enabling them to attend school and interact with classmates from afar.
The challenge going forward is finding where robots fit best in healthcare, and balancing the expectations with reality.
Dig Deeper:
Do Robots Have Value in Clinical Settings?
mHealth’s Promise: Mobility With Meaning
Origins of Robots in Healthcare
Taking a page from the retail industry in the late 1990s, healthcare first turned to robots to automate the supply chain. Guided by GPS technology, small and squat mobile units were designed to deliver supplies, replacing the need to dispatch a nurse or other staff member to restock cabinets.
"This new robotic breed is boasting features increasingly found in smartphones, gaming consoles and other consumer electronics, from advanced sensors and motion detectors to powerful microprocessors and voice activation,” the Wall Street Journal reported in 2012. “The service robots are self-aware, intelligent and able to navigate changing environments, even chaotic hospital settings."
Those robots, says Theobald, are designed to improve the supply chain and make the nurse’s life easier.
“The biggest cost in hospitals that people don’t think about is logistics,” claims Theobald, whose company produces the QC (Quality Care) Bot. “It can take up to about a third of your budget just getting the stuff you need and getting it to where it needs to be.”
“Nurses walk about five miles a day,” he explains. “That’s about a quarter to a third of their time. Imagine what would happen if we could cut down on that walking and allow them to do their jobs more efficiently.”
Two types of robots are generally found in this environment: supply and maintenance robots such as the QC Bot and Aethon’s Tugs robot, and mobile medical carts — often called computers-on-wheels or COWs. The latter are often dispatched to patient rooms to deliver patient orders or give doctors and nurses mobile access to medical instruments and the electronic medical record.
The first health systems to take full advantage of robots were pediatric hospitals that either ordered specially designed machines or dressed them up as characters to entertain their patients. More recently, these organizations used robots to help children adjust to the hospital and their care plan.
“There’s something important and almost magical about a robot,” Theobald observes. “Children will be much more open with them. It make a difference in their care.”
In California, Children’s Hospital of Orange County dispatched robots to Hoag Hospital Newport Beach to help with children admitted to the Emergency Department. The four-foot-tall robots enable CHOC pediatricians to assess the children — and talk to their parents — before transfer.
“The children think this technology is cool,” adds Jason Knight, MD, Medical Director of CHOC Children’s Emergency Transport Services, who uses his home computer, laptop, or iPad to use the robot. “When I introduce myself via the robot as a pediatric specialist, it always puts the parents’ minds at ease because from that point forward, CHOC is involved with their child’s care.”
Dig Deeper:
Factors Behind the Adoption of School-based Telehealth
Finding a Place for Real Time Location Systems in Healthcare

Source: ThinkStock
Many different uses for robots
Robots are actually showing up in several healthcare scenarios. A blog in Medical Futurist outlines the nine most common uses:
- Room disinfection. A robot using UV light can sterilize a room more efefctively than housecleaning, reducing the chances of a hospital-acquired infection like MRSA or C.diff.
- Reception. A robot can register patients, access medical records and provide detailed directions – in a y number of languages.
- Surgical assistance. Robotic arms, guided by a doctor, can perform basic surgical procedures in small or delicate areas, even when the doctor is miles away.
- Remote clinical encounters. Robots can serve as a doctor’s eyes and ears in clinics, community centers, retail locations and the patient’s home.
- Supply chain management. Robots can carry up to 400 pounds of supplies from one department to another, be programmed to respond to shortages, even deliver food and amenities to patient rooms.
- Assisting mobility-impaired patients. Some robots can assist patients getting in and out of beds or wheelchairs, while exoskeletons can improve mobility for patients with partial paralysis or other physical impairments.
- Drug delivery (think Fantastic Voyage, without the human cargo). Miniaturized robots can be deployed inside the body, delivering targeted doses of medication to specific locations, such as an organ or tumor.
- Blood drawing. Newly developed robots can pinpoint the ideal vein and withdraw blood in half the time it takes a nurse to do the same thing.
- Patient engagement. Robotic animals can help soothe the nerves of traumatized patients, especially children, or help them open up to care providers.
“As robots take care of our more intimate needs, such as personal caregiving, human to robot and robot to human interactions will become a central focus of study and philosophical discussion,” healthcare IT blogger Bernadette Keefe, MD, wrote in a 2016 post for the Mayo Clinic.
“There is much unknown regarding the ultimate acceptability of robots in intimate settings, or at work,” she concluded. “Comfort with robots may depend on multiple variables, such as the individual, culture, particular application, or industry. Trust is at the core of the use of autonomous robots in healthcare, and safety must be proven."
Dig Deeper:
Primary Care Telemedicine Produces High Patient Satisfaction
Top 10 Telemedicine Solutions by Hospital Site Implementations
Robots in critical care
In clinical settings, a robot can sometimes serve as the doctor’s representative, especially in cases where a specialist is required.
One of the first to be used in that setting was the RP-VITA, developed by iRobot (makers of the Roomba) and InTouch Technologies and given 501(k) clearance by the Food and Drug Administration in 2013. The five-foot-tall “autonomous navigation RP robot” was designed to combine mobility with an audio and video communication platform and instant access to patient medical records, as well as a navigation system that could map the environment for future reference and sense objects and people in its path.
"FDA clearance of a robot that can move safely and independently through a fast-paced, chaotic and demanding hospital environment is a significant technological milestone for the robotics and healthcare industries," iRobot Chairman and CEO Colin Angle said in 2013.
In one particular case, robots are proving their value. That’s in the emergency department, where a robot can connect patients and staff to a specialist miles away.
At Lompoc valley Medical Center, “Dr. Robot” is deployed in the Emergency Department to provide specialty care for stroke patients. Officially called a Remote Presence Virtual Independent Telemedicine Assistant, or RP-VITA, the five-foot-tall robot comes equipped with a high-definition video communications platform that allows the specialist to examine and communicate with the patient and on-site care team.
An April 2016 article in Lee Central Coast Newspapers describes how the telemedicine robot is used for someone suspected of suffering a stroke:
Once the patient is admitted, the hospital’s 12-member stroke alert team springs into action. This includes contacting the on-call neurologist, who is located in or near Los Angeles.
At the same time, the robot is dispatched from its docking station to the patient’s room.
The neurologist logs in through an encrypted connection, reviews the patient's scans and, using cameras attached to the robot, examines the patient, even zooming in to chekc the patient's pupils. He/she can also check data on bedside monitors and talk to both the patient and attending doctors and nurses.
“Because some crucial medications can be especially dangerous under certain circumstances, [Steven Reichel, MD, medical director of the LVMC emergency department] said it is nice having a specialist essentially in the room to provide an instantaneous second opinion, which becomes part of that patient’s medical record," the story notes.
One small hospital even credits robots with saving the facility from closing.
That’s the opinion put forth by Bryan Coffey, CEO of Hamilton County Hospital, a 25-bed critical care hospital in rural Kansas serving a population of about 2,700 people. In a 2014 white paper, Coffey said he took over the hospital in June 2013, when the hospital had no doctors, and immediately hired one physician and one cardiologist.
He then brought in an InTouch telemedicine robot.
“[We] started seeing a 180 (degree change). There’s been a 40 percent increase in (patient) volume and we’re consistently, month over month, 15 percent in growth,” Coffey told a local newspaper.
The hospital now uses the robot for ER as well as primary care visits and is adding service lines to connect patients through the robot to specialists, including dermatologists, pediatric doctors, and OB doctors.
“We have gone from a stagnant ‘stabilize and ship’ CAH to a vibrant provider of healthcare for our community … despite the fact that we are 55 miles from the nearest town with a Wal-Mart store,” Coffey wrote.
“The robot opens up opportunities for clinical affiliations which have increased interest from mid-level providers as well as some second and third year residents in medical school as they would no longer be the only town doctor,” he concluded. “We have gone from a hospital that was looking to close its doors in early 2013 to a vibrant growing and profitable hospital by 2014. So, if you are wondering how you can afford this robot, I would ask you how can you not afford to have this robot?”
Dig Deeper:
What Telemedicine, Telehealth Resource Centers Offer to Providers
Challenges, Opportunities of Mobile Health Devices in the Hospital
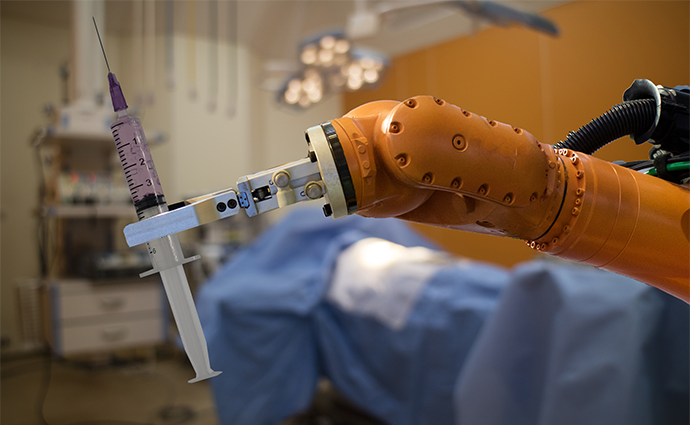
Source: ThinkStock
Robots in the operating room
Robots have been used to assist in delicate surgical procedures since 1985, when a robot surgical arm called the PUMA 560 was first used to perform a non-laparoscopic surgery.
The technology took a leap forward in 2000 with FDA approval of the da Vinci Surgical System, which has performed some 20,000 surgeries to date. In 2001, a team of New York-based physicians made history by using a robot named Zeus to perform a complete laparoscopic cholecystectomy on a patient in Strasbourg, France.
“It’s the same as if I were sitting in the operating room,” Mehran Anvari, a physician at St. Joseph’s Hospital in Hamilton, Canada who used the Zeus robot for more than 20 operations, including hernias and colon surgery, told BBC News in 2014. “I have both my hands on the robot the same way I would have instruments in both hands. … Basically, it’s the same as if I were next to the patient, just using telecommunication and robotics. It doesn’t feel different.”
Guided by the idea of using robots to perform surgeries in remote locations – such as space – healthcare providers and entrepreneurs have been working since then to refine the process.
In 2014, New York’s Mount Sinai Health System Icahn School of Medicine conducted two separate studies on the feasibility of telerobotics, with a doctor in one location controlling a robotic instrument in a surgical procedure at another site – ultrasounds in one study, echocardiogram exams in the other.
In the second study, Mount Sinai researchers collaborated with Kurt Borman, MD, of Umea University in Sweden to conduct robotic echocardiogram exams of several patients in remote clinics more than 100 miles from Borman's hospital.
According to Borman, the robot-assisted exams helped reduce diagnostic process time from 114 to 27 days, while a patient's wait time to see a specialist was reduced from 86 to 12 days; in addition, 95 percent of the patients involved in the remote consults said the results were superior to an in-person encounter.
"As a result of our pilot study, we were able to establish a safe and efficient e-health solution to improve the comprehensive, convenient examination of suspected heart failure patients in a rural community of northern Sweden and improve their physician care team's communication," said Narula, who published both studies in the August issue of the Journal of the American College of Cardiology-Imaging. "This pilot may serve as a future model for use of e-consults and robotic imaging in similar rural communities to improve access to specialists and the latest diagnostic technology globally."
And in 2015, the Florida Hospital Nicholson Center in Celebration conducted studies to determine if clinicians could conduct surgery via telemedicine. They found that while the technology is far more precise than it used to be, it’s not yet ready to sit in for the surgeon.
"The networks that exist today in well-equipped hospitals are more than capable of supporting telesurgery," Roger Smith, PhD, the Nicholson Centers Chief Technology Officer, said at the time. "But we've got a long way to go before that will happen."
Dig Deeper:
How Nighttime Telehealth Services Can Improve Overnight Care

Source: ThinkStock
Expectations and limitations
In 2011, Boston Children’s Hospital was one of several hospitals around the country to send robots home with newly discharged children in an early remote patient monitoring study. The robots, which cost roughly $6,000 apiece, were designed to interact with the children at home and enable caregivers to keep tabs on the kids’ health.
"Eventually, I see a whole fleet of these robots being sent home with patients,'' Hiep T. Nguyen, Associate Professor at Harvard Medical School and Children’s Director of Robotic Surgery Research and Training Center, told the Boston Globe. "With this technology, we're going to be able to replace hospital monitoring with home-based monitoring.''
It may be going there, but it hasn’t gotten there yet. Most of the programs were scrapped because the robots proved too expensive and didn’t provide enough clinical information back to caregivers to improve care management. In addition, providers are now looking at smaller, less invasive and more comprehensive RPM programs that use wireless devices and wearables.
“The pace of automation and robotics technology outruns the ability to get it into the hands of the clinicians,” Paul Sturrock, MD, a colon and rectal surgeon at UMass Memorial Medical Center and assistant professor at the University of Massachusetts Medical School, wrote in a 2016 blog. “In a healthcare environment, not only are the costs scrutinized -- the cost benefits are scrutinized even more. We are constantly evaluating these things and seeing what actually provides benefits to the patients and the advantages for doctors beyond being able to get their procedures done more efficiently.”
The upshot: Robots and robotics will work in certain situations where they provide services that reduce waste – both in time and money – help patients and improve workflows for doctors and nurses. As for the predictions that a robot might someday replace the doctor? Not just yet.
“We’ve all grown up with (robots) and we all believe they can do amazing and wonderful things,” iRobot Co-Founder and CEO Colin Angle pointed out during a panel discussion at the Digital Health Summit at the 2013 CES conference in Las Vegas, “but we always get ahead of ourselves.”
