Remote Patient Monitoring Brings mHealth Care Management Into the Home
With mHealth tools and platforms, remote patient monitoring programs have the potential to extend care management and coordination outside the doctor's office or hospital and into the patient's home.

Source: ThinkStock
Remote patient monitoring programs have the potential to reduce chronic care costs and hospital readmissions and improve clinical outcomes by moving care out of the hospital or doctor’s office and into the home.
Most of these programs focus on the collection of patient-generated health data from the home, through devices and mobile health platforms that connect to the primary care provider or care team. That data can either be collected and sent by the patient or gathered by connected devices and sent to the provider without the patient’s participation.
In this manner a provider can keep track of a patient around the clock, gathering data on health, activity, diet and exercise, the environment, even social determinants, thus filling out a health record that would otherwise focus on the patient’s visits to the doctor or hospital. By creating a more complete record, the provider can gain a better understanding of a patient’s overall health and develop a care plan that more closely adheres to a patient’s life.
A provider can also use the platform to push health and wellness advice, care management tips and other resources to the patient, based on trends spotted in RPM data. A diabetic patient consistently showing high blood sugar levels, for instance, might be urged to exercise more or alter his or her diet – or change his or her daily insulin intake to bring those readings down.
The path to acceptance for RPM devices and platforms hasn’t been easy. Providers have long been wary of remote monitoring technology for two reasons:
- Most of the technology hasn’t been proven reliable, leaving the doctor or nurse to wonder whether the data coming in from the patient is accurate enough to support a diagnosis or treatment plan.
- Devices and platforms that capture too much data threaten to overwhelm the provider with useless information.
Payers have been slow to reimburse providers for using the technology, as well, primarily because they haven’t seen proof that RPM is improving clinical outcomes. Researchers at Cedars-Sinai Medical Center reinforced that notion with a 2018 study pointing to a lack of data indicating that RPM produces long-term results.
“Despite anecdotal reports of RPM efficacy and growing interest in these new health technologies by researchers, providers, and patients alike, little empirical evidence exists to substantiate claims of its ability to improve clinical outcomes, and our research indicates many patients are not yet interested in or willing to share RPM data with their physicians,” the study concluded.
Ironically, Cedars-Sinai is one of several health systems across the country actively engaged in RPM pilot programs, so it may not take long for that earlier study to be revised.
- Banner Health’s Telehealth Program Cuts Hospitalizations and Costs
Remote Monitoring Platform is an mHealth Lifeline for New York’s ‘Sickest Children’
Use Cases for RPM
There are several potential use cases for remote patient monitoring. They include:
Chronic care management
Primary care providers can keep tabs on patients with chronic conditions in between office visits, promoting care management and intervening if data indicate a pending health issue.
Post-discharge care
Health systems are eager to keep track of patients after they’re discharged to make sure they follow their care plans and don’t experience setbacks that could lead to rehospitalization. In this scenario, the provider can also connect the patient with physical therapists and other specialists involved in rehabilitation.
Senior care
The growing numbers of seniors aging in place are putting pressure on providers to develop programs that connect to their older patients in their homes.
Workmen’s compensation cases
Payers, businesses and providers are all interested in tracking patients who have been injured on the job and are rehabilitating at home. All want to make sure they’re adhering to their care plan and are on a path to returning to work.
Behavioral health and substance abuse
.Providers treating these populations want to keep track of their patients outside the office to gain a better understanding of the social and environmental challenges affecting their health. An RPM platform can help providers identify health concerns and step in to address a potentially harmful issue, and they can be available in times of crisis. In addition, providers treating substance abuse issues can monitor their patients for relapses and ensure compliance in medication-assisted therapy (MAT) programs.
While hospitals and health systems generally view RPM as a means of engaging with a selected population of patients outside the hospital, smaller practices and even solo physicians can find value in the service to reduce unnecessary in-person visits, cut traffic in the waiting room, improve patient engagement and make sure patients don’t have to visit the hospital or doctor’s office for some emergency that could have been avoided.
Dig Deeper:
Can Remote Monitoring Keep COPD Patients Out of the Hospital?
Survey: Chronic Care Patients Want an mHealth Connection With Their Doctor

Source: ThinkStock
The Path Ahead for RPM
The rule of thumb in many healthcare IT implementations is that providers will begin using the technology if they’re reimbursed. That’s no different in the RPM arena, where payers – particularly the Centers for Medicare & Medicaid Services – have been wary of embracing devices and programs because they haven’t proven value.
Advocates see a vicious cycle: CMS won’t reimburse for RPM because there haven’t been enough pilot projects proving value, and providers aren’t launching RPM programs because they aren’t being reimbursed.
However, there are signs that CMS is changing its thinking on RPM.
In early 2018, CMS “unbundled” one of its more popular CPT codes for remote patient care, 99091. This action separated qualifying services from the agency’s restrictive telehealth and telemedicine reimbursement guidelines, which, among other things, prevent telehealth programs from being delivered to the patients’ home. This has opened the door for providers to be reimbursed for some RPM services, including data collection and care coordination.
More movement is expected soon. The American Medical Association, which creates CPT codes, has reportedly been working on several new codes that will create new opportunities for providers to use RPM devices and services. It will then be up to CMS to sanction those codes for reimbursement, or face pressure from an AMA that has grown more supportive of the technology.
CMS is facing pressure from two angles to be more accepting of RPM. Dozens of healthcare organizations and advocacy groups, including the Healthcare Information and Management Systems Society (HIMSS), College of Health Information Executives (CHIME), Center for Connected Health Policy (CCHP) and ACT | The App Association, have lobbied the agency to loosen its restrictions on both telehealth and RPM.
Congress, as well, has targeted CMS with dozens of bills, though few have completed the long journey to passage.
Dig Deeper:
CMS, AMA Look for Common Ground on Remote Patient Monitoring
GAO Report: Telehealth Troubles Tied to Reimbursement Barriers
Launching an RPM Program
When designing an RPM program, a provider needs to answer several questions:
Which patients should be monitored?
Select patients who have health issues that can be improved through home monitoring and who are open to being monitored at home. Complex cases might make it difficult to measure outcomes or success, and patients who aren’t fully on board will drop out of the program and drag the results down.
How long will the program last?
Most program begin with set deadlines, usually built around readmission rates and penalties. Some treatment programs may take longer. In chronic care, meanwhile, care management is often lifelong, so providers have to decide whether how to structure a program that continues as long as the patient does.
What data will be gathered?
Choose data – vital signs, activity, diet – that can be accurately and easily charted and used to effect clinical care decisions.
What devices will be used?
Select devices that are easy to use and reliable, and which can fit seamlessly into the patient’s home environment. Uncomfortable technology or clunky devices will be set aside and eventually ignored.
Who manages care coordination?
Design a workflow that makes the best use of office resources – nurses to handle the daily or weekly care coordination and management tasks, with doctors and specialists called in only when needed.
The challenge, as with any connected care initiative, is to lay the groundwork for success early, with a program that anticipates and meets goals rather than reacting to events.
It’s also important to remember that many mHealth and telehealth programs start slowly, often to the disappointment of their creators. Patient acceptance and engagement take time.
Dig Deeper:
Telehealth, RPM Help Visiting Nurses Fill Care Management Needs
Leveraging Primary Care Telehealth for Convenience and Quality
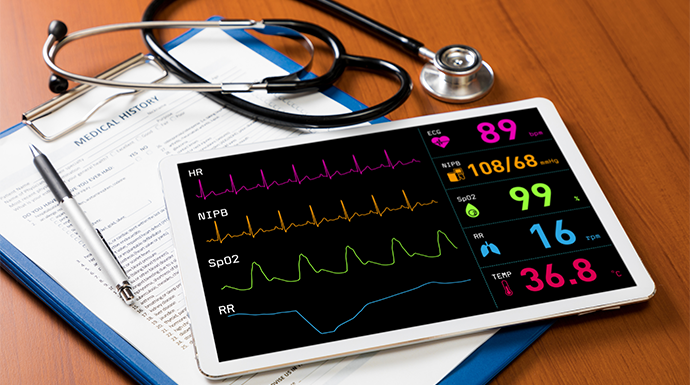
Source: ThinkStock
RPM and Consumer-Facing Technology
Consumer-facing technology, like fitness bands, smartwatches and connected home devices, would seem to have a natural fit in RPM programs. With a focus on style and comfort, they go a long way toward solving the patient engagement conundrum, saving providers the often time-consuming process of finding a device or service that the patient will like enough to keep using.
But many of these devices operate in a far different regulatory landscape than does healthcare technology – the vigorous design, testing and retesting undergone by clinical tools and devices isn’t matched in a commercial area where the focus is on making sure the product does what its marketing says it will do.
As a result, healthcare providers are wary of using them for clinical care and payers are reluctant to reimburse for their use.
Yet many of the top consumer brands, like Fitbit, Garmin, Apple and Samsung, are in use in many health systems around the country, including Boston’s Partners Healthcare, Ochsner Health in New Orleans and Los Angeles-based Cedars Sinai. In many instance, providers are using devices to collaborate with their patients on care management and coordination.
The idea behind many of these programs is that consumer-facing devices have value because they keep the patient engaged, and while the data they track and collect may not be accurate enough for clinical decision-making, they do allow providers to track health trends. For example, a fitness band or smartwatch might not be able to accurately gauge one’s blood-sugar level, blood pressure or heart rate, but several unhealthy readings in a row does indicate a trend and can indicate a pending health emergency.
Dig Deeper:
mHealth Finds a Place for Fitbit in Remote Patient Monitoring Research
KU Medical Center, Garmin to Analyze mHealth Value in Wearables
RPM and Medical Grade Data
For most connected care enthusiasts, the ideal RPM platform would include connected devices in the home automatically collecting and sending data to providers, without any active participation from patients. This would increase patient engagement and ensure that the information coming in to providers – clinical or medical grade data - is objective.
The market for clinical-grade devices is small but growing, fueled by companies like Philips, Honeywell and Ideal Life. In this arena the challenge is twofold: Develop a device that passes rigorous inspection, and make it seamless, intuitive and comfortable enough to be adopted by patients at home and used on a regular basis.
Another key component of the RPM platform is the IT framework that connects devices in the home with the care provider. Companies like Qualcomm Life and Validic specialize in this technology, creating hubs that pass data to cloud-based storage, where it is sorted and integrated with the electronic medical record and then presented to the care provider or care team.
These platforms don’t work, however, without input from the provider. Providers have to include rules-based engines that enable the provider to choose what data he or she wants to receive, then have that data not only streamed into the medical record but made quickly available on a dashboard for clinical use.
This is especially true in programs that enable providers to oversee care management for populations. A RPM platform, in this case, may present a high-level view of all patients being monitored, but it also enables the provider to drill down quickly to see which patients are falling outside care parameters and are in need on guidance.
Dig Deeper:
New mHealth Technology Platform Aims to Validate Remote Monitoring
Temple Launches Telehealth Program For Pulmonary Fibrosis Patients

Source: ThinkStock
Balancing RPM With the Bottom Line
In late 2017, a study issued by UPMC found that hospital and health systems are beginning to launch RPM programs regardless of reimbursement.
“Health systems are … balancing the remote monitoring investment with the potential for lost hospital revenue,” the study reports. “Many health systems note that investment is dependent on the systems’ at-risk population and connected to population health/value based care. As more patients are at-risk and the health system is financially responsible for the overall health of the total population, it will outweigh the lost hospital revenue.”
In Hudson, NY, for example, Columbia Memorial Hospital launched a small RPM program in late 2017, using grant money to create 50 RPM kits containing Bluetooth-enabled scales, blood pressure cuffs,pulse oximeters and an iPhone programmed with an RPM app.
“Sometimes these patients go home and they start deteriorating, but no one is around to pick up on that quickly enough, and we see them right back here,” says Dr. Ronald J. Pope, medical director of CMH Care Centers and the program’s director.
Pope says roughly 20 percent of discharged patients end up back in the hospital within 30 days due to complications that could have been avoided had the hospital been able to monitor those patients at home. For a typical hospital, those readmissions will cost the hospital between $500,000 and $1 million in penalties.
He figures the program will pay for itself if it can reduce hospitalizations by at least one-third.
“We’re kind of at the cutting edge of these projects,” he says, estimating that the health system is now about 20 percent value-based and 80 percent fee-for-service. “We want to reduce costs, but we’ll need data to demonstrate value.”
In cases of chronic care management, healthcare providers have to think about how to create a program that can follow the patient through the course of his or her life. In some cases this means shifting to a subscription- or insurance-based model.
“A lot of what we’re looking for is to empower these people and keep them out of the hospital,” said David Taylor, RN, telehealth services supervisor for the Visiting Nurse Association of the Rockford Area, part of Rockford Health, which developed a subscription-based RPM program in 2016. “They need to be in charge of (their health management) … when we’re not there anymore.”
That may be the ultimate goal for any RPM program: to create a mindset in the patient that he or she can live a healthier life by paying more attention to exercise, diet and other daily habits – with occasional guidance from one’s care provider.
With the development of the “smart home” concept and the Internet of Things and the advent of better mHealth technology, remote patient monitoring stands to become an accepted standard of care. The promise of RPM lies in its potential to bring care management and coordination into the home and make health and wellness an integral part of life.
